Study Reveals Uniquely Human Gene Enhancing Immune Function

UB researchers are finding that the active form of this gene promotes a broad range of protective traits
BUFFALO, N.Y. – The University at Buffalo team that discovered how a gene found in 75% of us protects against neurodegeneration has now found that this same gene enhances immune function as well.
The new findings were published in eBioMedicine online before print on April 2.
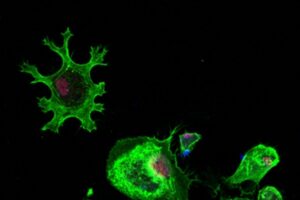
CHRFAM7A is a uniquely human gene that occurred after humans split from a common ancestor with chimpanzees millions of years ago.
The gene has been implicated and studied in neuropsychiatric disorders, and the UB team’s previous work identified how the gene is protective against memory disorders, such as Alzheimer’s Disease, but its role in immune function has not been well understood.
Kinga Szigeti, MD, PhD, corresponding author, professor of neurology in the Jacobs School of Medicine and Biomedical Sciences at UB and a physician with UBMD Neurology, says the team wasn’t surprised to find that the gene has an immune-enhancing function.
Immune advantage
“We always thought that the fact that this mutation is enriched in the human population–meaning that since it helped people survive, more and more people became carriers–indicated that it would provide an immune advantage,” she says.
The research reveals how it does that and it turns out to be related to the team’s previous work.
Last year, the UB team published a study showing that the active form of the CHRFAM7A gene allows brain cells to be more flexible. That work showed that it does this by activating actin cytoskeleton, which provides structural support to cells, allowing brain cells to be more resilient. That property provides protection against neurodegenerative diseases such as Alzheimer’s.
Now the team has found that the gene’s activation of actin cytoskeleton also enhances immune function. “Our research shows that as human cells evolved with their cytoskeleton, they gained new function, allowing them easier access to fight sources of infection in the body,” says Szigeti.
She explains that CHRFAM7A changes calcium signalling in the cell, the cell’s most ancient signal transduction system (i.e. communication system).
“That signalling change leads to a switch in how the actin is organized, producing cells that are tougher on the outside, creating a stronger, better shield, which is called lamellipodia,” explains Szigeti.
Cutting through the matrix
The CHRFAM7A cells have an additional immune advantage. “The immune system needs a road to get into infected tissue,” she adds, “and the CHRFAM7A cells developed a new mechanism: they can cut through the extracellular matrix or fabric of the organs and get to places that have limited vascularization or have been compromised by disease.”
Since this advantage allows immune system cells to get into the infected tissue more efficiently, the infection can be controlled earlier, leaving the bacteria or the virus limited time to replicate, she continues.
Because of the gene’s impact on calcium signalling, which is a key driver of numerous fundamental biological processes, including cellular metabolism, it likely also affects many other biological and pathological processes.
Uniquely human genes endow people with human-specific traits; Szigeti notes that traditional animal models of diseases, which lack these genes, cannot therefore accurately reflect how some drugs will function in humans.
“So far, it’s clear that the active form of CHRFAM7A provides protection against multiple disorders,” says Szigeti. “This research could lead to the identification of important new drug targets.”
To do the current study, the team used pluripotent stem cells that have the mutation through genetic engineering.
“We used human cells that can be differentiated into the first responders of the immune system (monocytes) and tested how they can get into engineered substrates that model human tissue stiffness in health and disease,”
she said.
So far, the gene has been implicated in the systemic inflammatory response, inflammatory bowel disease (IBD), COVID-associated cytokine storm, HIV-associated neurocognitive disorders, osteoarthritis and cancer metastasis.
The UB team is currently testing the gene’s role in the human brain, IBD and cancer metastasis.
Co-authors with Szigeti include faculty and postdoctoral fellows from the Department of Neurology, the Department of Physiology and Biophysics and the Clinical Translational Science Institute in the Jacobs School, and Roswell Park Comprehensive Cancer Center.
Partial funding was provided by the Community Foundation for Greater Buffalo and in part by the National Institutes of Health.







