Prostate MRI for Cancer Evaluation: Invaluable Information for Patients at Risk
by David Cipolla, M.D.
The prostate is a small walnut-shaped gland in males that produces the seminal fluid that transports sperm. After skin cancer, prostate cancer is the most common type of cancer in men. Many prostate cancers grow slowly without causing serious harm, but others are more aggressive and may spread quickly. Diagnosing prostate cancers as early and accurately as possible is critical.
Even aggressive prostate cancer often has no symptoms until the disease is advanced. Screening may help detect cancer early, but there is no one-size-fits-all approach. Most prostate cancer screening begins with a prostate-specific antigen (PSA) blood test and digital rectal exam (DRE). PSA is a protein produced by normal, as well as malignant, cells of the prostate, and is often elevated in prostate cancer patients. However, screening tests are not 100 percent accurate — conditions, such as benign prostatic hyperplasia (BPH) and prostatitis can also cause an abnormal PSA test or DRE.
When there is a clinical concern for underlying prostate cancer, a biopsy is advised, which can cause bleeding, pain, and infection. Prostate biopsies traditionally comprise random samples of the prostate. With this approach, cancerous areas may be missed, or insignificant cancers detected, while more aggressive cancer elsewhere in the gland may not be sampled and identified.
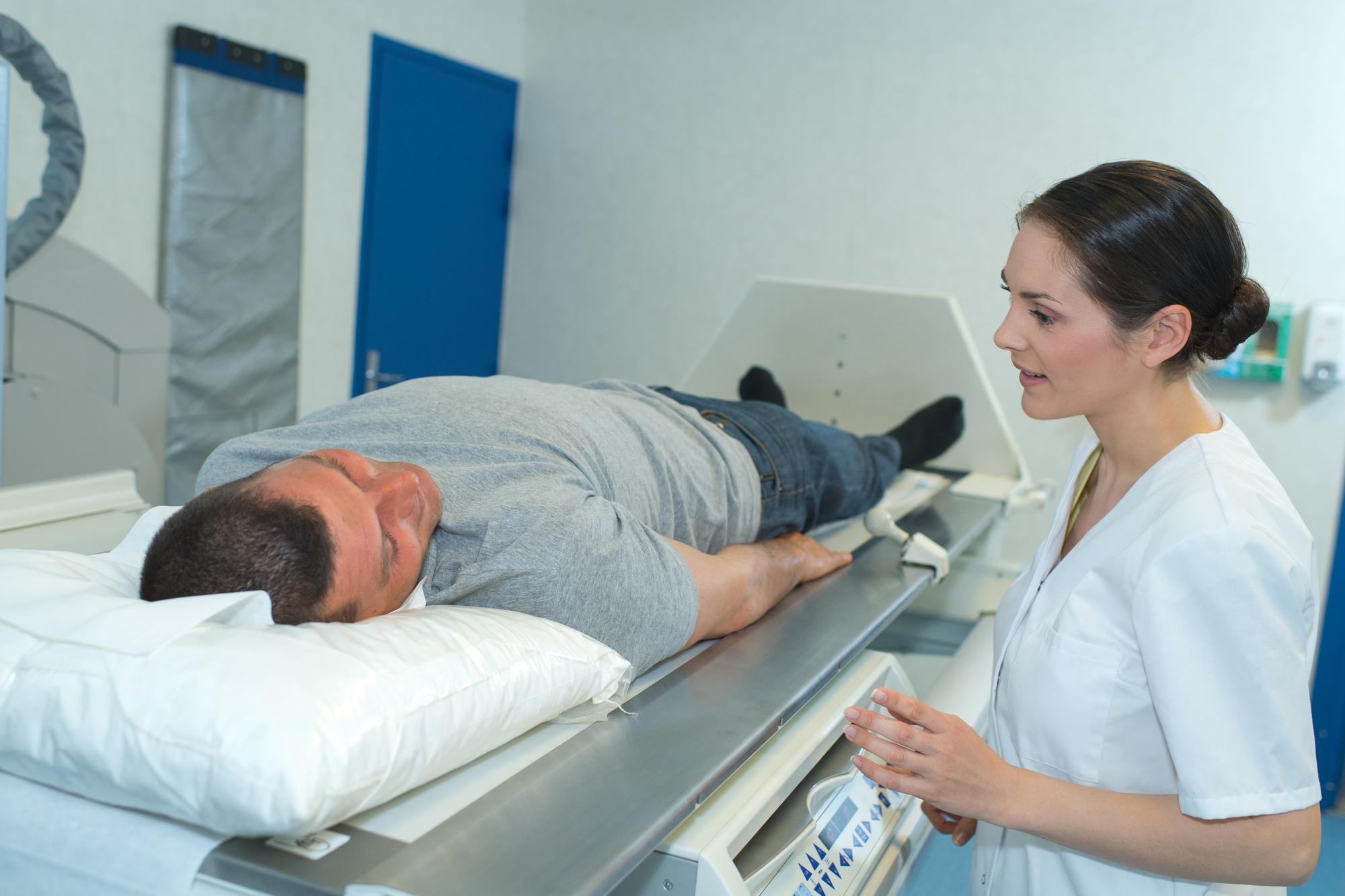
Prostate MRI (magnetic resonance imaging) is a powerful tool to aid clinical decision making and optimally detect and stage prostate cancer. MRI utilizes magnetic and radio waves to produce highly detailed images of soft tissue structures in the body, such as the prostate. Patients who undergo an MRI lie flat on a table that is slid into an MRI machine. The scan is completed in about 30 minutes. Intravenous contrast material is often utilized to optimize the exam which requires a small IV in the arm. The procedure is otherwise non-invasive.
A prostate MRI can provide invaluable information regarding the internal structure of the prostate and detect suspicious areas. This assists the provider, often a urologist, in determining whether or not a biopsy is appropriate when the diagnostic information derived is combined with the patient’s PSA level, risk factors, and age. If a prostate MRI demonstrates no suspicious findings, it can be reassuring for the patient and clinician. If there is a suspicious lesion, the subsequent biopsy can be targeted to this area utilizing technology which highlights the area of abnormality in real time for the urologist performing the procedure.
The good news is that even aggressive prostate cancer is highly treatable when detected early. It is important for men to be evaluated by experts who utilize the most advanced techniques, such as prostate MRI, to ensure an accurate and timely diagnosis. Patients at risk for prostate cancer should ask their clinician if this test is appropriate for them. In general, discussions with your doctor should begin in your 40s.
David Cipolla, M.D., a radiologist practicing at Great Lakes Medical Imaging (GLMI). If you are at risk for prostate cancer, talk with your provider about having your exam at GLMI. Call 716-836-4646 to make an appointment, and visit www.greatlakesmedicalimaging.com.







